Root canal therapy represents one of the most misunderstood procedures in dentistry, often accompanied by anxiety about both the treatment process and associated costs. For patients facing potential endodontic treatment, the financial implications can be substantial, with procedures ranging from several hundred to several thousand dollars depending on complexity and location.
The decision to proceed with root canal therapy involves multiple factors that extend beyond immediate pain relief. Treatment success depends on proper diagnosis, appropriate timing, and realistic expectations about outcomes. Patients who approach this decision without adequate information frequently encounter unexpected complications, additional procedures, or results that fall short of their expectations.
Understanding the key questions to ask before committing to treatment helps patients make informed decisions while avoiding common pitfalls that can lead to significant financial and health consequences. The complexity of endodontic procedures means that initial consultations often fail to address critical concerns that emerge during or after treatment.
Understanding Treatment Necessity and Alternatives
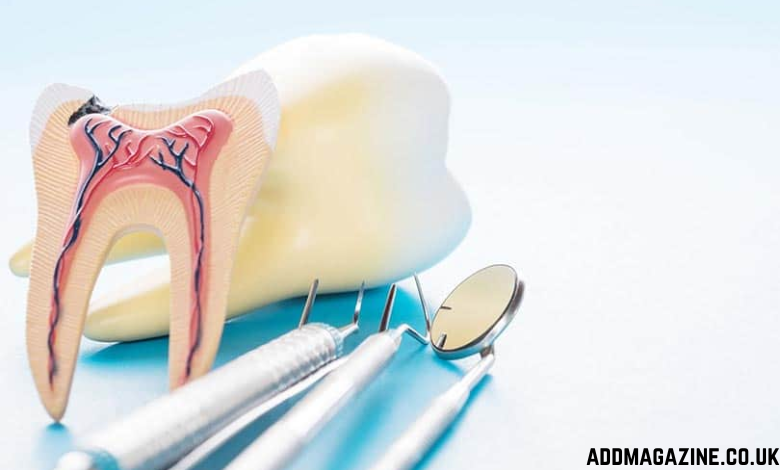
Root canal therapy becomes necessary when the pulp inside a tooth becomes infected or severely damaged, typically due to deep decay, repeated dental procedures, or trauma. However, not every tooth experiencing discomfort requires immediate endodontic intervention. Affordable care dental services root canal therapy options exist, but understanding when treatment is truly necessary prevents unnecessary procedures and associated costs.
The distinction between reversible and irreversible pulpitis determines whether conservative treatments might suffice or whether root canal therapy represents the only viable option for tooth preservation. Reversible pulpitis often responds to less invasive treatments, while irreversible pulpitis typically requires either endodontic treatment or extraction.
Diagnostic Accuracy and Second Opinions
Accurate diagnosis requires comprehensive evaluation including clinical examination, symptom assessment, and appropriate radiographic imaging. Cold testing, percussion testing, and palpation help determine pulp vitality and the extent of infection or inflammation. However, diagnostic accuracy varies among practitioners, and symptoms can sometimes be misleading.
Seeking a second opinion becomes particularly important when diagnosis remains unclear or when symptoms don’t align clearly with clinical findings. Endodontists possess specialized training in diagnosing complex cases and may identify alternative treatment approaches that general dentists might not consider.
Alternative Treatment Considerations
Extraction followed by replacement options represents the primary alternative to root canal therapy. Dental implants, bridges, and partial dentures each offer different advantages and limitations compared to preserving the natural tooth through endodontic treatment.
The long-term cost comparison between root canal therapy and tooth replacement often favors preservation, particularly when considering the potential need for future maintenance or replacement of prosthetic devices. However, teeth with poor structural integrity or extensive bone loss may not justify the investment in endodontic treatment.
Evaluating Treatment Complexity and Success Probability
Root canal complexity varies significantly based on tooth anatomy, number of roots and canals, presence of calcifications, and extent of infection. Anterior teeth typically present fewer complications than molars, which may have multiple roots and complex canal systems that challenge even experienced practitioners.
Pre-treatment evaluation should include assessment of root anatomy through appropriate imaging, evaluation of periodontal health, and consideration of restorative requirements following endodontic treatment. Teeth requiring extensive restoration may need crown lengthening or other adjunctive procedures that add to overall treatment cost and complexity.
Anatomical Complications and Technical Challenges
Calcified canals, curved roots, and accessory canals can significantly complicate treatment and reduce success rates. Advanced imaging techniques help identify these challenges before treatment begins, but some complications only become apparent during the procedure itself.
Procedural complications such as instrument separation, perforation, or inability to locate all canals may necessitate referral to an endodontist or consideration of surgical intervention. Understanding these possibilities before treatment helps patients prepare for potential additional costs and extended treatment timelines.
Success Rate Expectations and Long-term Prognosis
Success rates for root canal therapy vary depending on multiple factors including pre-treatment diagnosis, tooth location, practitioner experience, and patient factors such as immune response and oral hygiene. Initial treatment success rates generally range from 85% to 95%, but long-term success depends heavily on adequate final restoration.
Teeth that have undergone endodontic treatment require prompt placement of permanent restorations to prevent recontamination and structural failure. Delayed restoration represents one of the most common causes of treatment failure, yet patients often underestimate the importance of timely follow-up care.
Financial Planning and Insurance Considerations
Root canal therapy costs vary significantly based on tooth location, treatment complexity, geographic region, and practitioner fees. Front teeth typically cost less to treat than premolars, which cost less than molars. Additional procedures such as retreatment, surgical intervention, or post placement increase overall expenses.
Insurance coverage for endodontic procedures varies widely among plans, with some covering basic treatment while excluding more complex procedures or retreatment. Understanding coverage limitations before treatment prevents unexpected out-of-pocket expenses and allows for appropriate financial planning.
Hidden Costs and Additional Procedures
The quoted fee for root canal therapy often represents only the endodontic portion of treatment. Additional costs may include temporary and permanent restorations, posts or buildups for structural support, and crowns for long-term protection. Emergency visits, pain management, and potential retreatment add further expense.
Some patients require sedation or specialized procedures that increase treatment cost. Referral to an endodontist typically involves higher fees but may be necessary for complex cases or when complications arise during initial treatment.
Payment Options and Treatment Timing
Many dental practices offer payment plans or financing options that make treatment more accessible. However, delaying treatment due to cost concerns can lead to more complex and expensive procedures if infection spreads or tooth structure deteriorates further.
Emergency treatment often costs more than scheduled procedures, and limited appointment availability may result in temporary measures that add to overall treatment expense. Planning treatment during non-emergency periods typically provides more options for managing costs and selecting appropriate practitioners.
Practitioner Selection and Treatment Setting
The choice between treatment by a general dentist versus an endodontist affects both treatment outcomes and costs. General dentists handle routine cases effectively, while endodontists specialize in complex procedures and possess advanced equipment for challenging cases.
Practitioner experience with specific types of cases influences success rates and complication frequency. Asking about case volume, continuing education, and referral patterns helps patients evaluate practitioner qualifications for their specific situation.
Technology and Equipment Considerations
Modern endodontic treatment benefits from advanced technology including digital imaging, rotary instrumentation, and microscopic visualization. These technologies can improve treatment outcomes and patient comfort, but may not be available in all practice settings.
The availability of cone beam computed tomography (CBCT) imaging allows for better diagnosis and treatment planning, particularly in complex cases. Practices with limited imaging capabilities may need to refer patients for specialized imaging, adding to treatment time and cost.
Emergency Access and Follow-up Care
Post-treatment complications can occur even with successful procedures, making access to emergency care an important consideration. Practices with limited emergency availability may leave patients without adequate support during critical healing periods.
Follow-up care requirements include monitoring healing progress, placement of permanent restorations, and long-term evaluation of treatment success. Understanding these requirements and associated costs helps patients plan for complete treatment rather than just the initial procedure.
Post-Treatment Expectations and Long-term Care
Recovery from root canal therapy typically involves temporary discomfort that resolves within several days to weeks. However, some patients experience prolonged sensitivity or discomfort that may indicate complications requiring additional treatment.
The treated tooth requires permanent restoration within a reasonable timeframe to prevent recontamination and structural failure. Temporary restorations provide short-term protection but cannot withstand long-term chewing forces or prevent bacterial infiltration indefinitely.
Restoration Requirements and Crown Necessity
Most teeth requiring root canal therapy need crown coverage for long-term success, particularly posterior teeth that experience significant chewing forces. The additional cost of crown placement should be factored into treatment planning from the outset.
Some anterior teeth with minimal structural loss may not require crown coverage, but this determination depends on remaining tooth structure and functional requirements. Conservative restorations may suffice in select cases, but patients should understand the increased risk of future fracture.
Long-term Monitoring and Maintenance
Endodontically treated teeth require periodic evaluation to monitor healing and detect potential complications. Routine radiographic examination helps identify developing problems before they become symptomatic and require more extensive treatment.
Signs of treatment failure may not appear immediately, with some complications developing months or years after initial treatment. Regular dental visits allow for early detection and intervention when problems arise, potentially avoiding more complex and expensive procedures.
Conclusion
Root canal therapy represents a significant investment in oral health that requires careful consideration of multiple factors beyond immediate cost. Success depends on accurate diagnosis, appropriate treatment planning, skilled execution, and proper follow-up care. Patients who ask the right questions before committing to treatment position themselves to make informed decisions that align with their health needs and financial capabilities.
The complexity of endodontic procedures means that initial consultations should address not only the immediate treatment requirements but also long-term expectations and potential complications. Understanding these factors helps prevent costly mistakes and ensures that patients receive appropriate care for their specific situations.
Taking time to thoroughly evaluate treatment necessity, practitioner qualifications, and financial implications ultimately leads to better outcomes and greater satisfaction with the treatment process. The questions outlined provide a framework for these important discussions and help patients avoid the common pitfalls that can turn necessary dental treatment into expensive complications.